
Cách Chọn Người Đồng Hành Hỗ Trợ Tâm Lý Phù Hợp: Tiêu Chí, Câu Hỏi Nên Hỏi Và Dấu Hiệu Cần Đổi
Choosing the right psychological support companion isn’t about finding someone “perfect.” It’s about finding someone safe, skilled, and compatible with your goals—so you can make steady progress without feeling judged, rushed, or stuck. ✅
If you’ve been searching for cách chọn người đồng hành hỗ trợ tâm lý phù hợp: tiêu chí, câu hỏi nên hỏi và dấu hiệu cần đổi, this guide translates that intent into a practical, US-friendly decision framework: clear criteria, smart questions to ask, and red flags that mean it’s time to switch. 🧠

What “psychological support companion” can mean (and why it matters)
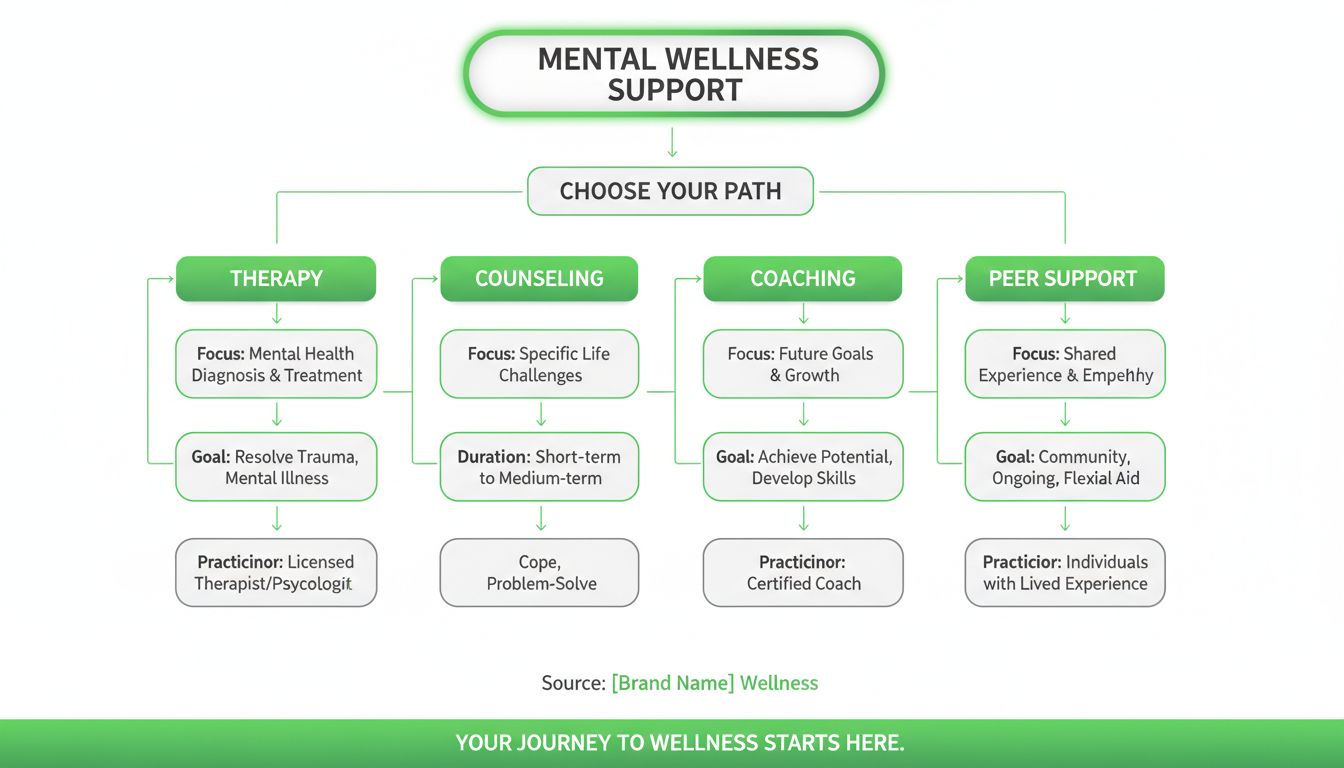
In practice, “support companion” can describe different roles:
- Therapist (licensed): diagnosis, treatment planning, evidence-based psychotherapy.
- Counselor: structured talk support, coping skills, life transitions (credentials vary by state).
- Coach: goal setting, accountability, performance and behavior change (not mental health treatment).
- Peer supporter: lived experience support, community-based encouragement (not clinical care).
Let’s be honest: confusion here is a silent progress-killer. If you expect trauma therapy but hire a life coach, you’ll feel misunderstood. If you want accountability but book open-ended talk therapy, you might feel like you’re “venting” forever.
If you want a clear comparison before you decide, read Coaching vs psychological counseling—what to choose and when.
Start with your goal: what do you want help doing?
Before you evaluate any person, define your outcome in plain language:
- “I want fewer panic spikes and better sleep.”
- “I want to stop spiraling after conflict.”
- “I want to rebuild after burnout and not relapse.”
- “I want to process grief without shutting down.”
- “I want tools for boundaries and self-worth.”
Then choose the “support lane”:
| Your primary need | Best-fit support type | What success looks like |
|---|---|---|
| Persistent anxiety, depression symptoms, trauma, OCD, eating concerns | Licensed therapy (or supervised clinician) | Symptom reduction + functioning improves |
| Stress, life transition, relationship patterns | Counseling/therapy | Better coping + clearer choices |
| Goals, performance, confidence, habits | Coaching | Action plans + consistent follow-through |
| Belonging, shared experience, recovery community | Peer support | Reduced isolation + practical hope |
If you’re unsure whether what you’re feeling is “serious enough,” use a fast self-check: Signs of depression in adults and how to self-screen.
The non-negotiables: 7 criteria for a safe, effective match
These criteria matter more than vibe. Chemistry is important—but ethics and competence come first.
1) Appropriate training and scope ✅
You should be able to understand:
- What they’re trained in (degrees, licenses, certifications)
- What they do and don’t treat
- When they refer out
If they imply they can treat everything, that’s not confidence—that’s a warning.
2) Evidence-based methods (not just “talking”)
A good support companion can name their approach in simple words:
- CBT, ACT, DBT skills, attachment-based work, trauma-informed care, somatic tools, mindfulness-based interventions, etc.
You don’t need jargon. You need a method you can track.
3) Clear structure: goals, plan, and markers of progress
Ask yourself: do you leave sessions knowing what you’re working on next week?
Healthy structure often includes:
- A shared goal
- A plan (even if flexible)
- Homework or experiments (when appropriate)
- Regular check-ins on outcomes
4) Psychological safety and respect
You should feel:
- Heard without being “handled”
- Challenged without being shamed
- Free to disagree
Safety doesn’t mean comfort 100% of the time. But it does mean you’re not afraid of being punished for honesty.
5) Cultural fit and values alignment
This is the big one. Your beliefs about family, identity, religion, gender roles, boundaries, and autonomy affect the work.
You’re not looking for someone identical to you. You’re looking for someone who can hold your context with respect.
6) Boundaries and ethics 🧩
A professional has:
- Clear confidentiality rules and limits (harm to self/others, abuse reporting requirements depending on jurisdiction)
- Transparent fees, cancellations, communication policy
- No pressure, no manipulation, no dependency-building
7) Logistics that reduce friction (so you actually show up)
Because practical barriers kill consistency:
- Scheduling ease
- Time zone compatibility
- Online vs in-person fit
- Session frequency you can sustain
For a deeper breakdown, read Online therapy vs in-person therapy—how to choose.

The best questions to ask before booking (and what good answers sound like)
You don’t need to interrogate them. But you do need clarity. Use these questions like a filter.
Questions about fit and experience
- “Have you worked with concerns like mine?”
Good answer: specific themes + what tends to help + honest limits. - “What approach do you use, and why?”
Good answer: plain-language explanation + examples. - “How do you define progress?”
Good answer: measurable changes (sleep, rumination, behavior, relationships) + check-ins.
Questions about structure and process
- “What does a typical session look like?”
Good answer: a predictable flow (check-in → focus → skills/insight → next steps). - “How long do people usually work with you?”
Good answer: ranges, not guarantees—and a willingness to review. - “Do you give practices between sessions?”
Good answer: optional, tailored, not punitive.
Questions about safety and boundaries
- “What are your confidentiality limits?”
Good answer: clear and confident. - “How do you handle it if I feel worse after a session?”
Good answer: normalization + stabilization tools + plan adjustments. - “What if I disagree with you or want to change direction?”
Good answer: welcomes feedback, collaborative stance.
Questions about logistics and accessibility
- “What’s your cancellation and rescheduling policy?”
- “Do you offer online sessions? What platform?”
- “How can I contact you between sessions (if at all)?”
Here’s a fast “copy/paste” pre-screen checklist you can use:
| Category | Ask this | You’re listening for |
|---|---|---|
| Competence | “What training supports your work with my issue?” | Specific credentials + scope |
| Approach | “What methods do you typically use?” | Clear, evidence-based, flexible |
| Progress | “How will we track improvement?” | Outcomes + review points |
| Safety | “How do you handle crises or escalation?” | Plan + referrals + boundaries |
| Fit | “What’s your style—directive or exploratory?” | A style that matches you |
| Logistics | “What frequency do you recommend to start?” | A realistic plan you can sustain |
Green flags: signs you found a good match 🌿
Look for these patterns over the first 2–4 sessions:
- You feel more clear after sessions (even if emotional).
- They summarize your words accurately and check: “Did I get that right?”
- They help you name emotions and needs without labeling you.
- You leave with one useful takeaway—a skill, a reframe, or a next step.
- They respect your pacing (especially with trauma and shame).
- They welcome feedback: “Let’s adjust.”
- You feel more agency, not more dependence.
Red flags: when “not a fit” becomes “not safe” 🚩
Not every mismatch is harmful. But some are.
Mild mismatch (try a conversation first)
- You don’t like their style (too quiet / too directive).
- Sessions feel vague or repetitive.
- You’re unsure about goals.
Often fixable with a direct request: “Can we set a clearer plan and track progress?”
Serious red flags (consider switching quickly)
- They shame you, mock you, or dismiss your feelings.
- They break confidentiality casually.
- They push their personal ideology as “the answer.”
- They discourage you from seeking medical care when needed.
- They blur boundaries (flirting, gifts, dependence cues, excessive messaging without structure).
- They make big promises: “I can cure you in X sessions.”
- You consistently feel worse with no stabilization plan.
Crisis-level red flags (stop and get support immediately)
- They suggest anything unsafe, coercive, or illegal.
- They ignore self-harm risk or don’t have a crisis protocol.
- They retaliate when you question them.
If you’re in immediate danger or thinking about harming yourself, contact 988 (US Suicide & Crisis Lifeline) or emergency services.
The “switching” playbook: how to change support without losing momentum
Switching can feel like failure. It isn’t. It’s precision.
Step 1: Name the problem in one sentence
Examples:
- “I don’t feel emotionally safe bringing up my real thoughts.”
- “We don’t have goals or progress markers.”
- “Your approach doesn’t fit what I need right now.”
Step 2: Request a repair conversation (if it feels safe)
Use a simple script:
- “I want to keep working together, but I need more structure and clear goals. Can we try that for the next 3 sessions and review?”
If they respond defensively or blame you, that’s information.
Step 3: Decide with a time box
Give it 2–4 sessions with a specific change request. No improvement? Switch.
Step 4: Ask for a referral or summary
A professional can provide:
- A brief summary of goals worked on
- Helpful notes on what interventions were used
- Referral suggestions
Step 5: Keep one stabilizing routine while transitioning
Consistency reduces backsliding. If anxiety is spiking, pair the transition with grounding tools:
- Try this guide: Breathing and grounding exercises to reduce anxiety at home
How to choose between online and in-person—without overthinking it
A lot of people get stuck here. The takeaway is clear: choose the format you’ll actually attend consistently.
| Factor | Online support | In-person support |
|---|---|---|
| Convenience | Highest (no commute) | Lower (travel time) |
| Comfort | Home environment helps some | Neutral space helps others |
| Access | Easier for rural/busy schedules | Better if privacy at home is hard |
| Body-based work | Possible, depends on provider | Often easier to facilitate |
| Consistency | Often higher | Can drop with logistics |
If privacy is your issue, consider:
- Headphones + white noise
- Sitting in a parked car
- Booking at times when home is quiet
Mini self-assessment: what style of support works best for you?
Choose the statements that feel most true:
- “I want practical tools and homework.” → skills-based, structured approach (CBT/ACT/DBT-informed)
- “I need to process deep patterns and relationships.” → attachment/psychodynamic-informed support
- “My body goes into fight/flight.” → trauma-informed + somatic tools
- “I’m overwhelmed and exhausted.” → burnout recovery pacing + boundary work
If burnout is part of your story, you’ll likely benefit from a paced recovery plan: What to do when you’re burned out—signs, causes, and a 7-day reset plan.

Where Ngọc Tĩnh - Hỗ Trợ Tâm Lý fits (and how to explore options)
Ngọc Tĩnh - Hỗ Trợ Tâm Lý is built to help you make informed choices—whether you’re looking for a steady companion for emotional support, practical coping strategies, or a structured journey with accountability.
You can:
- Explore the available offering: View the “Đồng Hành Cùng Tiên” service details
- Browse more resources and self-guided learning: Read the mental wellness blog
- Reach out with your questions and preferences: Contact Ngọc Tĩnh - Hỗ Trợ Tâm Lý
Quick recap: your decision checklist ✅
Use this as your final filter:
- Role fit: Are you choosing therapy vs coaching vs peer support correctly?
- Competence: Can they clearly explain training, scope, and approach?
- Safety: Do you feel respected, not shamed?
- Structure: Do you have goals and progress markers?
- Fit: Does their style match what you need right now?
- Boundaries: Are policies clear and professional?
- Switch signals: If it’s not improving after a time-boxed repair attempt, you’re allowed to change.
The right psychological support companion won’t “save” you. They’ll help you build the skills, insight, and stability so you can carry yourself—with support that feels steady, ethical, and human. 🤝
