
Khi Nào Nên Tìm Hỗ Trợ Tâm Lý: Dấu Hiệu Sớm Của Lo Âu, Stress Kéo Dài Và Khủng Hoảng Cảm Xúc
If you’re Googling “khi nào nên tìm hỗ trợ tâm lý: dấu hiệu sớm của lo âu, stress kéo dài và khủng hoảng cảm xúc”, you’re probably already past the “I’m fine” stage. And that’s not dramatic—it’s practical. Most people don’t wake up and search for mental health support on a great day.
This guide helps you answer one core question: When should you get psychological support? You’ll learn the early signals of anxiety, the red flags of chronic stress, and the urgent signs of an emotional crisis—plus what to do next. 🧠

Quick answer: When should you seek psychological support?
You should consider support when your emotional state starts to impair your life, when coping tools don’t work anymore, or when symptoms persist long enough that they become your “new normal.”
Here’s the simplest decision rule:
- If it’s affecting your sleep, relationships, work, appetite, or sense of safety for more than 2 weeks, support is reasonable.
- If you feel unsafe (self-harm thoughts, panic that feels unmanageable, dissociation, violent impulses), it’s urgent—seek immediate help. 🚨
- If you’re functioning but suffering, don’t wait for a breakdown. Early support is often faster, gentler, and more effective.
The takeaway is clear: you don’t need to be “at your worst” to deserve help.
A practical “signal chart”: mild vs. moderate vs. urgent
Sometimes the hardest part is labeling what’s happening. Use this table to sort what you’re feeling into a level of action.
| Level | What it tends to look like | What you should do next |
|---|---|---|
| Early / mild | Worry spikes, irritability, low motivation, trouble unwinding, mild sleep issues | Start skills + monitor for 7–14 days; consider a consult if it repeats |
| Moderate / persistent | Symptoms most days, avoidance, frequent conflict, productivity drop, physical stress symptoms | Schedule support; build a plan and accountability |
| Urgent / crisis | Self-harm thoughts, panic attacks that feel out of control, substance escalation, hopelessness, inability to function | Seek immediate help locally; don’t stay alone |

Q&A: Early signs of anxiety you shouldn’t ignore 😰
Anxiety isn’t just “worry.” It often shows up as body symptoms, mental loops, and behavior changes long before you call it anxiety.
1) “Is it anxiety if I can’t stop thinking about worst-case scenarios?”
Yes—especially if you notice:
- Replaying conversations and imagining what you “should’ve said”
- Catastrophizing (jumping from small uncertainty to disaster)
- Feeling relief only briefly, then the worry returns
If reassurance-seeking becomes a habit (asking others, Googling symptoms, checking messages repeatedly), that’s a strong early cue.
2) “My body feels anxious, but my mind says I’m fine—what’s that?”
That’s common. Anxiety often speaks through your nervous system:
- Tight chest, shallow breathing
- Stomach issues, nausea, IBS flares
- Headaches, jaw clenching, muscle tension
- Racing heart, restlessness, sweaty palms
When your body is stuck in fight-or-flight, you can feel “on edge” even without a clear reason.
3) “How do I know it’s not just stress?”
Stress typically has a trigger you can name (“deadline,” “money,” “conflict”). Anxiety can persist even when the trigger is gone—or expand to many areas (“everything feels risky”).
If you’re unsure, you don’t have to diagnose yourself. You just need to notice: Is it shrinking your life? (avoiding places, people, decisions, or opportunities)

Q&A: Signs your stress is no longer “normal” (chronic stress) 😵💫
Let’s be honest: being busy isn’t the issue. Being chronically dysregulated is. Chronic stress is when your system never fully returns to baseline.
4) “How long is ‘too long’ to be stressed?”
A rough guideline: if stress symptoms last most days for 2–4 weeks and you’re not recovering with rest, weekends, or small self-care efforts, it’s no longer just a rough patch.
5) “What are the early warning signs of stress that’s turning chronic?”
Look for patterns like:
- Sleep changes: trouble falling asleep, waking at 3–4 a.m., nightmares
- Emotional changes: irritability, crying easily, numbness, feeling “flat”
- Cognitive changes: brain fog, forgetfulness, decision fatigue
- Behavior changes: withdrawing, doomscrolling, overeating/undereating
- Relationship changes: snapping, avoiding conversations, feeling misunderstood
6) “My performance is fine—but I feel awful. Does that count?”
Yes. High-functioning stress is real. If you’re “doing well” while internally burning out, support isn’t a luxury—it’s prevention.
If burnout is a concern, you’ll likely relate to the patterns described in this burnout recovery guide.

Q&A: Emotional crisis—what it looks like (and what to do) 🚨
A crisis isn’t always loud. Sometimes it’s quiet: numbness, shutdown, or the feeling that you can’t keep going like this.
7) “What counts as an emotional crisis?”
Common crisis markers include:
- Feeling hopeless, trapped, or like you’re a burden
- Panic attacks or fear spikes that disrupt daily life
- Dissociation (feeling unreal, detached, “not in your body”)
- Sudden rage, impulsivity, or risky behavior
- Increase in substance use to cope
- Inability to do basics: eating, showering, leaving bed, responding to messages
8) “When is it urgent enough to seek immediate help?”
If you have:
- Thoughts of self-harm or suicide
- A plan or intent to harm yourself
- You feel you cannot stay safe
- You’re experiencing hallucinations, paranoia, or severe disorientation
In the US, you can contact 988 (Suicide & Crisis Lifeline) for immediate support. If you’re in immediate danger, call 911 or go to the nearest ER.

The “2-week rule” and other fast self-checks
You don’t need perfect clarity. You need a workable checkpoint.
The 2-week rule ✅
Consider support if for 2+ weeks you’ve had one or more:
- Sleep disruption
- Appetite changes
- Persistent worry or dread
- Loss of interest/joy
- Frequent irritability or tears
- Avoidance and withdrawal
- Physical stress symptoms (headaches, stomach issues, tension)
The “cost” question
Ask yourself:
- What is this costing me daily—energy, time, relationships, confidence?
- What opportunities am I avoiding because of how I feel?
- If nothing changes in 3 months, would I be okay with that?
If the honest answer is “no,” that’s your cue.

Common myths that keep you stuck (and the truth)
These are the mental traps that delay care—sometimes for years.
| Myth | Reality |
|---|---|
| “I should handle it myself.” | Self-reliance is great—until it becomes isolation. Support is a tool, not a weakness. |
| “Other people have it worse.” | Pain isn’t a competition. If you’re struggling, it matters. |
| “If I start therapy, it means I’m broken.” | Therapy is often skill-building, emotional processing, and nervous system regulation—not “fixing” you. |
| “I’ll wait until it gets really bad.” | Early support often prevents crises and shortens recovery time. |

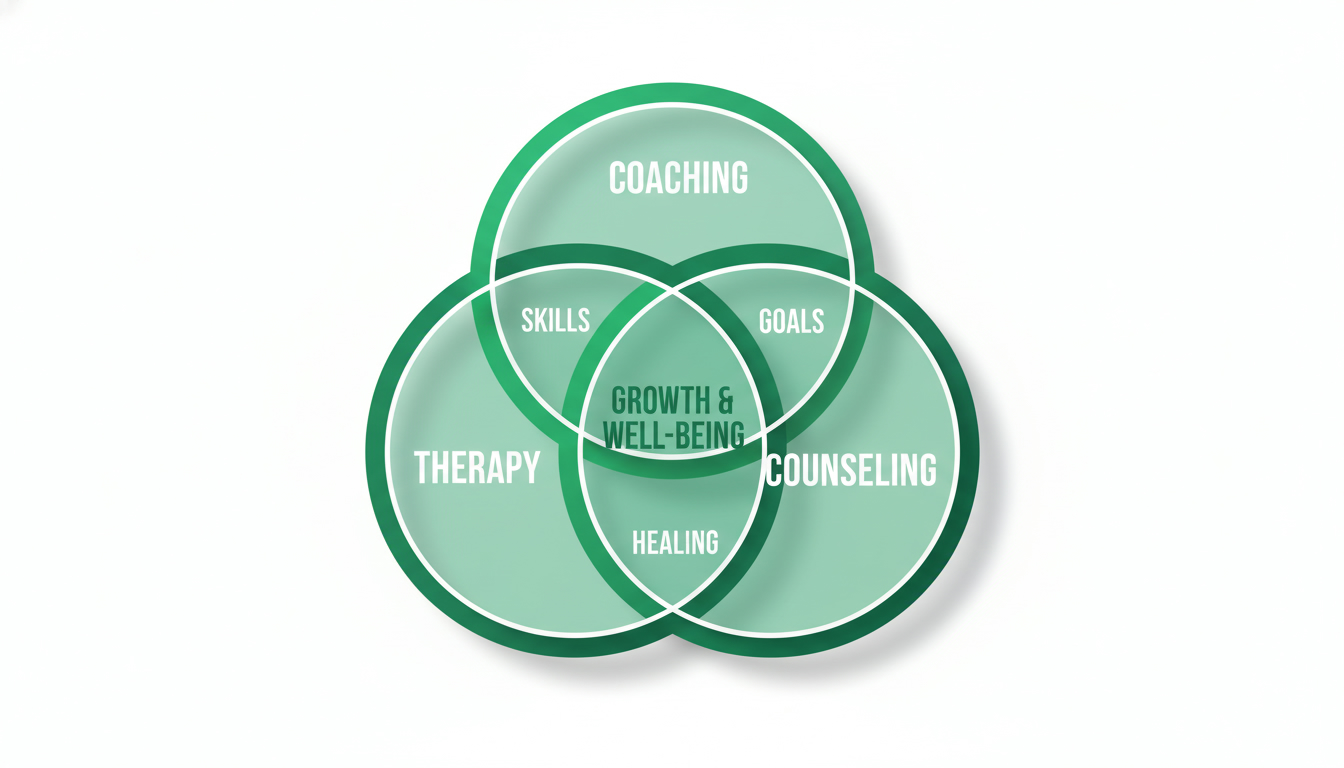
What kind of support should you seek? (Therapy vs coaching vs counseling)
This part matters because “support” isn’t one-size-fits-all.
If you’re debating options, this breakdown will save you time: therapy vs coaching—what’s the difference and when to choose each.
Here’s a simplified decision table:
| Your main need | Often a good fit |
|---|---|
| Anxiety/stress symptoms, emotional triggers, coping skills | Therapy or structured psychological support |
| Identity, direction, habits, performance goals | Coaching (sometimes alongside therapy) |
| Relationship conflict patterns, communication breakdown | Therapy / counseling support |
| Trauma symptoms, panic, dissociation, severe depression | Trauma-informed therapy and clinical care |
What to expect in your first sessions (so it feels less scary)
New support can feel intimidating. Here’s what usually happens:
- You explain what’s been going on (symptoms, triggers, history—only what you’re ready to share).
- You clarify goals: sleep, anxiety reduction, boundaries, emotional regulation, relationship stability.
- You and your supporter set a plan: frequency, methods, small weekly actions.
If you want a deeper guide on picking the right person, use this checklist for choosing a mental health companion/supporter.

What you can do today (even before you book) 🌿
Support works best when you combine sessions with simple, repeatable skills.
Start with:
- One nervous system reset per day (breathing, grounding, short walk)
- One boundary action (say no, delay a response, block focus time)
- One connection (text a trusted person, ask for company, don’t isolate)
If anxiety is spiking right now, practice a structured technique from this grounding and breathing guide for anxiety relief.

When you’re ready: how to reach Ngọc Tĩnh - Hỗ Trợ Tâm Lý
If you want structured support—especially for early anxiety, chronic stress, or emotional overwhelm—you can explore services and book a next step with Ngọc Tĩnh - Hỗ Trợ Tâm Lý.
- Learn what’s available via Ngọc Tĩnh’s support services
- Reach out directly using the contact page to schedule support
FAQs: the most searched questions about getting psychological support
“How do I know I’m not overreacting?”
If your reaction is persistent, distressing, and interfering, it’s not “too much.” It’s information—your system asking for care.
“What if I don’t know what to talk about?”
You don’t need a perfect story. Start with:
- What you’re struggling with this week
- What you’re avoiding
- What you wish felt easier
“How soon should I seek help after a major life event?”
If you’ve experienced a breakup, job loss, grief, health scare, or family conflict and notice sleep disruption, panic, numbness, or shutdown lasting more than 2 weeks, it’s a strong time to get support.
“Can support help even if I’m not diagnosed?”
Yes. Most people seek help for symptoms and life impact, not diagnoses.
If you remember one thing: you don’t need permission to get help. If anxiety is getting louder, stress isn’t lifting, or your emotions feel unmanageable, support is a smart next move—not a last resort.
