
Dấu Hiệu Trầm Cảm Ở Người Trưởng Thành Và Cách Tự Kiểm Tra Ban Đầu
You’re not “weak” for wondering whether what you’re feeling might be depression. You’re paying attention. And that’s a big deal. 🧠
This guide breaks down dấu hiệu trầm cảm ở người trưởng thành và cách tự kiểm tra ban đầu (signs of depression in adults and how to do an initial self-check) in a clear, non-alarmist way—so you can name what’s happening, reduce confusion, and know what to consider next.

What “depression in adults” actually looks like (beyond feeling sad)
Let’s be honest: adult depression often doesn’t show up as “crying all day.” It can look like:
- You’re functioning—working, parenting, replying to messages—but everything feels heavy
- You’re “fine” on paper, yet nothing feels enjoyable
- You’re exhausted, but sleep doesn’t refresh you
- You keep thinking you should be grateful, but your body says otherwise
Clinically, depression (major depressive disorder) is typically a cluster of symptoms affecting mood, thinking, body, and behavior—lasting most days for at least 2 weeks, and causing noticeable distress or impairment.
Core signs of depression in adults (the “big two” + the common set)

The “big two” symptoms clinicians watch for
Many diagnostic frameworks start with these two:
- Persistent low mood (sad, empty, numb, or irritable)
- Loss of interest/pleasure (things you used to like now feel flat)
If one (or both) of these is present, the next step is to look for additional patterns below.
Common emotional & cognitive signs
- Feeling hopeless, worthless, or excessively guilty
- Harsh self-talk: “I’m failing,” “I’m a burden,” “Nothing will change”
- Trouble concentrating, making decisions, or remembering details
- Feeling emotionally “shut down” (numbness can be depression too)
Physical and behavioral signs (often missed)
- Changes in sleep: insomnia, early waking, or sleeping much more
- Changes in appetite/weight (up or down)
- Low energy, moving slowly, or feeling “dragged down”
- Restlessness or agitation (especially in adults who don’t present as sad)
- Withdrawing socially, ignoring calls/texts, canceling plans
- Reduced productivity, increased mistakes, or “bare minimum” survival mode
Depression can also show up as irritability
In adults—especially those under chronic stress—depression can look like:
- Snapping quickly
- Feeling constantly overwhelmed
- Zero patience for small problems
That doesn’t mean you’re “a bad person.” It can mean your nervous system is overloaded.
Depression vs. stress vs. burnout (why it’s easy to confuse them)
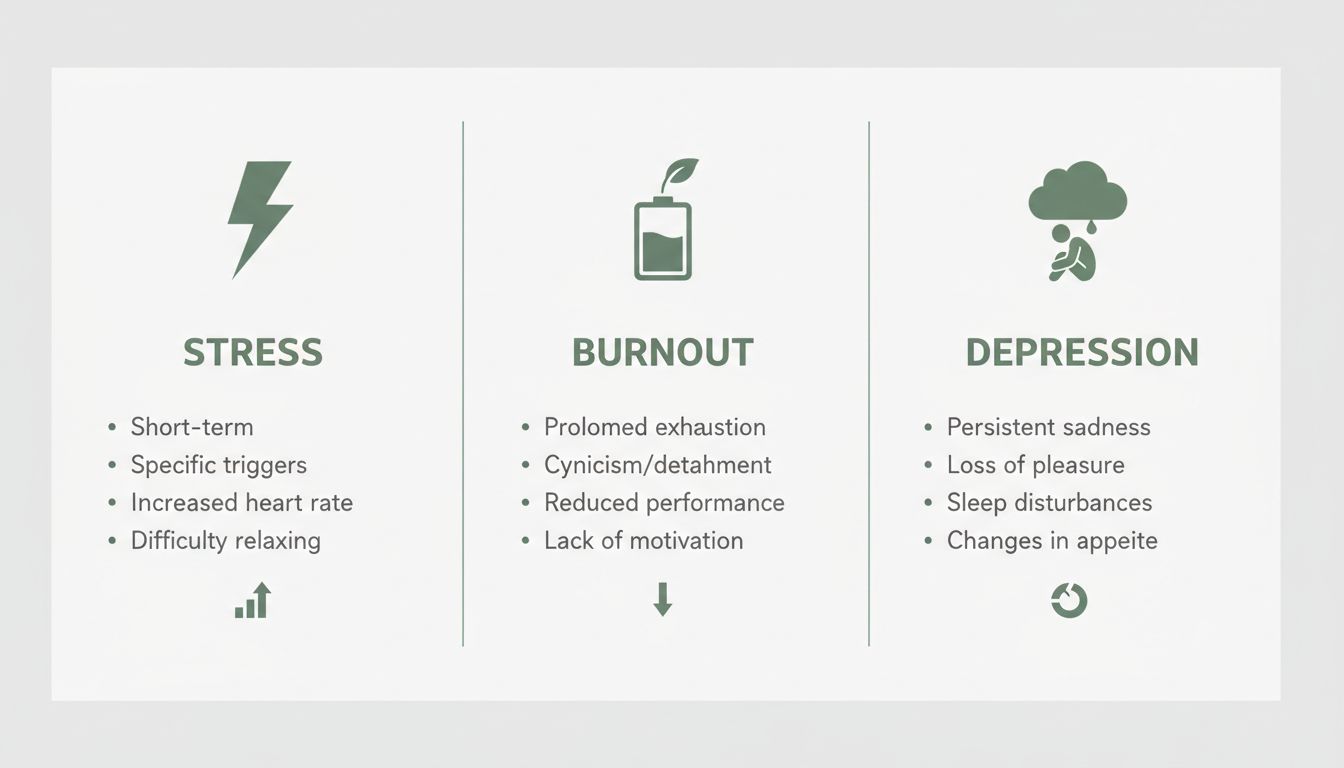
Stress, burnout, and depression overlap—so you need a few clean distinctions.
| Pattern | Stress | Burnout | Depression |
|---|---|---|---|
| Primary driver | Ongoing pressure | Prolonged overload (often work/caregiving) | Mood disorder pattern (multi-factor) |
| Mood | Anxious, tense | Cynical, depleted | Empty, hopeless, numb, or irritable |
| Motivation | Still present (but strained) | Drops mainly around the stress source | Drops broadly across life |
| Pleasure | Can still enjoy breaks | Harder to enjoy work-related things | Enjoyment fades even in “good” moments |
| Body | Hyperarousal (tense, restless) | Exhaustion, “nothing left” | Sleep/appetite/energy shifts, slowed or agitated |
| Self-view | “I can’t keep up” | “I can’t do this anymore” | “I am the problem / there’s no point” |
If you want a deeper breakdown, read Stress vs depression: how to tell the difference and respond appropriately.
The initial self-check: what to notice (without diagnosing yourself)

A good “first check” isn’t a test you pass or fail. It’s a pattern check across time, intensity, and impact.
1) Time: has this been going on most days for 2+ weeks?
- Depression is less about a single bad day and more about persistence
- If symptoms have lasted months, that’s even more important to acknowledge
2) Intensity: is this feeling “stuck,” not shifting with rest?
Ask:
- When you get a break, does your mood rebound at least a little?
- Or does the heaviness follow you everywhere?
3) Impact: is it interfering with daily functioning?
Look at:
- Work/school performance
- Relationships
- Basic self-care (showering, meals, cleaning)
- Decision-making and problem-solving
4) Breadth: is it affecting multiple areas of life?
Burnout can be localized (e.g., mostly work). Depression is often broader:
- hobbies feel pointless
- socializing feels like effort
- even small tasks feel impossible
5) Risk signals: any thoughts about not wanting to exist?
If you’re having thoughts like:
- “I wish I could disappear”
- “People would be better off without me”
- “I can’t do this anymore” …treat that as a serious signal, not a shameful secret. You deserve support.
The takeaway is clear: a self-check is about spotting patterns—then choosing a next step that reduces risk and increases support. ✅
A simple “symptom snapshot” table you can use today
Use this as a quick mirror. Mark what’s been true most days lately.
| Area | What to look for | Yes/No (most days) |
|---|---|---|
| Mood | low, empty, numb, or irritable | |
| Interest | loss of pleasure/interest | |
| Energy | fatigue, heaviness, low drive | |
| Sleep | too little/too much/poor quality | |
| Appetite | increased or decreased | |
| Thinking | guilt, hopelessness, self-criticism | |
| Focus | poor concentration/decision fatigue | |
| Movement | slowed down or restless | |
| Social | withdrawal, isolation | |
| Function | trouble with work/home tasks |
If several boxes are “Yes,” and it’s affecting your life, that’s a strong cue to consider professional support—not because you’re broken, but because you shouldn’t have to carry it alone.
What an online screening can (and can’t) tell you
Here’s the honest truth: online questionnaires can be useful, but they’re not a diagnosis.
What they can do
- Give language to what you’re experiencing
- Estimate symptom severity
- Help you decide whether to seek assessment/support
What they can’t do
- Rule out medical causes (thyroid issues, anemia, sleep disorders, medication effects)
- Capture context (grief, trauma, relationship dynamics, workplace harm)
- Replace a full evaluation
If you want to explore support formats, you may find this helpful: Online therapy vs in-person therapy: how to choose what fits you.
Why adults often miss depression in themselves (and what to watch for)

Adult depression is frequently masked by responsibility. You might tell yourself:
- “I can’t fall apart—I have people counting on me.”
- “Other people have it worse.”
- “I’m just tired. It’ll pass.”
But depression can be high-functioning for a long time—until it isn’t. Common “masked” patterns include:
- Overworking to avoid feelings
- Doom-scrolling late at night because silence feels unbearable
- Emotional eating or loss of appetite
- Constant self-criticism disguised as “motivation”
- Increased alcohol/cannabis use to numb out 🍷 (even mild increases matter if it’s coping)
When it’s time to talk to a professional (clear thresholds)

Consider reaching out if any of these are true:
- Symptoms persist 2+ weeks and are interfering with life
- You feel hopeless, stuck, or emotionally numb most days
- Sleep/appetite changes are significant
- You’re withdrawing and can’t “snap out of it”
- You’re using substances more to cope
- You’ve had thoughts about self-harm or not wanting to live
If you want structured support with a compassionate guide, explore Ngọc Tĩnh’s support services with Tiên. If you’re ready to ask questions or discuss fit, you can also get in touch through the contact page.
What to expect from support (so it feels less intimidating)
People avoid reaching out because they imagine therapy/coaching will be awkward or judgmental. A good support process is usually:
- Collaborative: you set goals together
- Practical: you work with thoughts, routines, boundaries, and emotion regulation
- Validating: your experience is taken seriously (without dramatizing it)
- Individualized: not one-size-fits-all
If you’re unsure what type of support matches your needs, this comparison can clarify it: Coaching vs psychological counseling: differences and when to choose each.
Frequently asked questions (adult depression self-check)

“If I’m still working and functioning, can it still be depression?”
Yes. “High-functioning depression” isn’t a formal diagnosis, but it describes a real pattern: you keep going externally while internally feeling flat, exhausted, or hopeless.
“What if I’m not sad—just numb?”
Numbness, disconnection, and lack of pleasure are common depressive presentations. Not feeling sad doesn’t mean you’re fine.
“Could this be bipolar disorder instead?”
If you have periods of unusually elevated energy, decreased need for sleep, impulsivity, racing thoughts, or risky behavior alternating with lows, it’s worth screening for bipolar spectrum conditions with a professional.
“Is self-checking enough?”
Self-checking is a starting point—useful for clarity, not for certainty. If your symptoms are persistent or impairing, a professional assessment is the next rational step.
Key takeaways you can hold onto today
- Adult depression often shows up as exhaustion, numbness, irritability, and loss of pleasure—not only sadness.
- The initial self-check is about time (2+ weeks), intensity, impact, and breadth across life areas.
- If you’re experiencing hopelessness, shutdown, or thoughts of not wanting to exist, you deserve support now—not later. 🤝
If you want more mental health education and gentle, practical reflections, you can browse Ngọc Tĩnh’s blog library.
